Breast Screening
The NHS Breast Screening Programme aims to identify breast cancer in asymptomatic (no symptoms), apparently healthy women. The aim is early detection where treatment is more successful with a good chance of recovery.
This screening service has been running since 1988, inviting all women aged 50-70 years for mammograms (x-ray of the breast) once every three years. The rationale for screening this age group is that the majority of breast cancers occur in women aged 50 and above. In the UK, over 1.3 million women are screened each year diagnosing about 10,000 breast cancers – with almost 75% of those invited attending their assessment. Since 2007, an age extension has enabled women aged 47-73 to access breast screening.

Feeling a lump, change in size or shape?

Breast screening across the world varies with some countries offering mammograms every year from the age of 40 years to others not having any screening programmes. In the UK, different screening protocols are offered to women considered to be at an increased risk of developing breast cancer – for example women at high risk of developing breast cancer (i.e. BRCA1 and BRCA2 carriers) may be offered annual MRI scans.
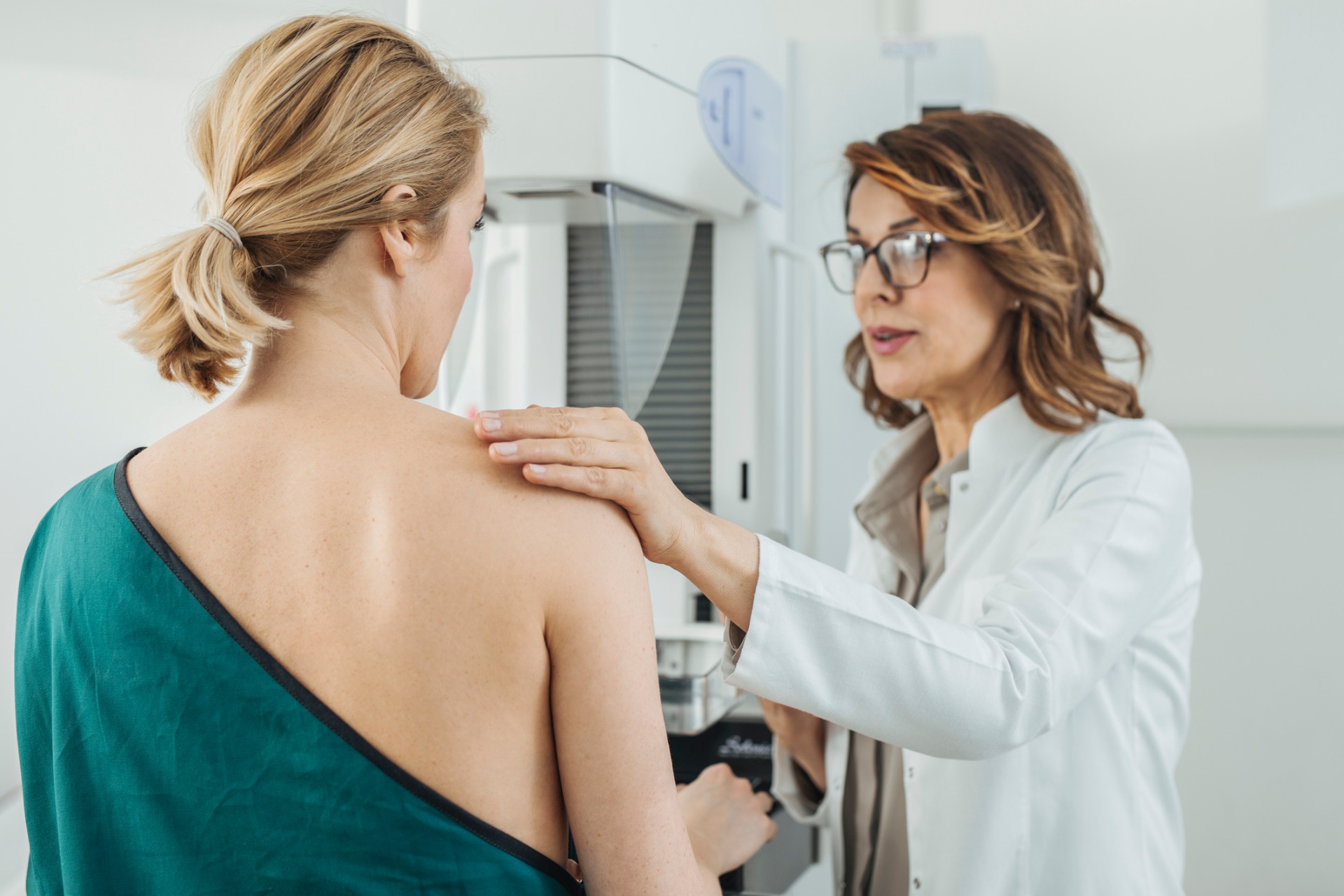
For the vast majority breast screening involves attending a breast clinic or a mobile screening unit. A health practitioner (mammographer) will undertake the mammograms and will assess any special health considerations including pregnancy, breastfeeding, breast implants and disability. The mammographer will usually take 2 x-rays of the breast – one from above and one from the side. Some women find this an uncomfortable procedure but compression of the breast tissue is required to ensure a good quality mammogram covering as much breast tissue is taken.
RESULTS
Results are available within 2 weeks – the vast majority of women (96 out of 100) are notified about a satisfactory result with no obvious signs of cancer found. These women (according to age) will be invited to further screening mammograms in 3 years. A small number of women (4 out of 100) will be recalled for further tests that may include a biopsy. Ultimately, 1 out of 4 of those with an abnormal screening result will be diagnosed with breast cancer.
PREVENTION
Controversy surrounding breast screening includes the potential harms of over-diagnosis and whether ultimately there is a survival benefit. An independent review in 2012 calculated that for every 10 000 UK women aged 50 years invited to screening for the next 20 years, 43 deaths from breast cancer would be prevented and 129 cases of breast cancer, invasive and non-invasive, would be over-diagnosed; that is one breast cancer death prevented for about every three over-diagnosed cases identified and treated.




